Technology enablers and key drivers
The key technology enabler that has accelerated this transformation during the pandemic is the wide availability of connectivity technology, which can be either wired (e.g., Ethernet) or wireless (e.g., Bluetooth, Wi-Fi, cellular). The latter is especially appealing because it provides greater mobility, and as we will explain later, more security. Coupled with the changes made to Current Procedural Terminology (CPT) codes by the Centers for Medicare and Medicaid Services, RPM has become an attractive solution for healthcare providers to improve patient care and generate additional revenues.
In addition to the pandemic, population aging and chronic diseases have also altered the public mindset about remote healthcare. Not too long ago, the United Nations did a study which found that the number of people worldwide who are 65 and older will increase from 703 million in 2019 to 1.5 billion by 2050, for an increase of 120%. The Bookings Institute also found that the number of Americans over age 55 grew by 27% between 2010 and 2020, which is 20 times larger than the growth rate of the collective population under 55 (1.3%).
Regarding chronic diseases, also known as noncommunicable diseases (NCDs), which include cardiovascular diseases (such as heart attack and stroke), cancers, chronic respiratory diseases (such as chronic obstructive pulmonary disease and asthma), and diabetes, the World Health Organization estimated that they kill 41 million people each year. This is equivalent to 71% of all deaths globally. Today, chronic diseases not only represent the leading cause of illness and death, but they also significantly impact the quality of life for those suffering from them. With longer life expectancy and more disposable income, there is naturally a growing demand for solutions that can improve the quality of life and greater independence for the elderly and for all patients.
Always-on, Always Connected
For HDOs and medical device manufacturers (MDMs), this growing demand gives rise to connected medical devices for remote patient monitoring (RPM) and chronic care management (CCM). As connectivity brings more mobility, these medical devices can provide an always-on, always-connected experience for their users. For healthcare providers and doctors, these mobile RPM devices provide better accuracy and immediacy of patient health data. Since regular monitoring is an essential part of any successful disease management program, physicians, healthcare providers, and patients themselves can get a more holistic view of patients’ vital statistics around the clock. The end result is the transformation of the healthcare industry from episodic and reactive patient care programs to those that are preventative and outcome-based.
Private health info brings high value
While connectivity and mobility technologies provide many benefits, there are also certain risks that need to be carefully managed. The chief of them is information security. After all, what is valuable to patients and the healthcare providers is also valuable to malicious actors. Specifically, the average price of a person’s medical record on the dark web can fetch between $250 to $500. In contrast, the average price of credit card or social security information is only $1. The main reason for this disparity is that while credit card information and even social security numbers can be changed when fraud is committed, a person’s private health information, or PHI, can include health records, health histories, lab test results, and medical bills. This set of info does not change and is persistent over time. And it could be used for submitting fraudulent claims.
This is why cybersecurity breaches hit an all-time high in 2021 for the healthcare industryi. According to IBMii the average cost of a cybersecurity breach in the healthcare industry has risen from a staggering $7.13M in 2020 to $9.23M in 2021. Based on the U.S. Department of Health and Human Services Office for Civil Rights’ breach portaliii, the number of breaches, specifically those resulting in the release of unsecured protected health information affecting 500 or more individuals, has gone up. The majority of these breaches is due to hacking and IT incidents. The accompanying table shows the data from the last four years.
| Year | 500+ breaches reported | Individuals Affected | Hacking / IT Incident |
| 2021 | 715 | 49,824,243 | 75% |
| 2020 | 656 | 37,641,403 | 68% |
| 2019 | 408 | 38,732,966 | 57% |
| 2018 | 302 | 12,196,601 | 42% |
Cellular technology is ideal for RPM
In terms of security, while Wi-Fi and Bluetooth are two low-cost wireless connectivity options supported by most mobile RPM devices, their biggest drawbacks are poor security enforcement and inconsistency in the connectivity setup process for end users. Either one could result in an unpleasant setup experience for the user or other security issues for the manufacturer.
With cellular connectivity, however, MDMs can streamline and simplify the user experience for all their connected RPM devices. The freedom and flexibility to have connectivity solution providers select and manage the best coverage wherever the RPM device is located in the world make a lot of business sense. First and foremost, it frees the MDMs from the headache of connectivity management to focus their attention and resources on delivering the best customer experience through product innovations.
Moreover, low-power wide-area (LPWA) cellular technology can provide the following key benefits that rivals Wi-Fi and Bluetooth cannot:
- Global coverage
- Ideal for high-mobility use cases
- Low-power consumption
- Strong cybersecurity protection
- Optimized for large-scale IoT deployments
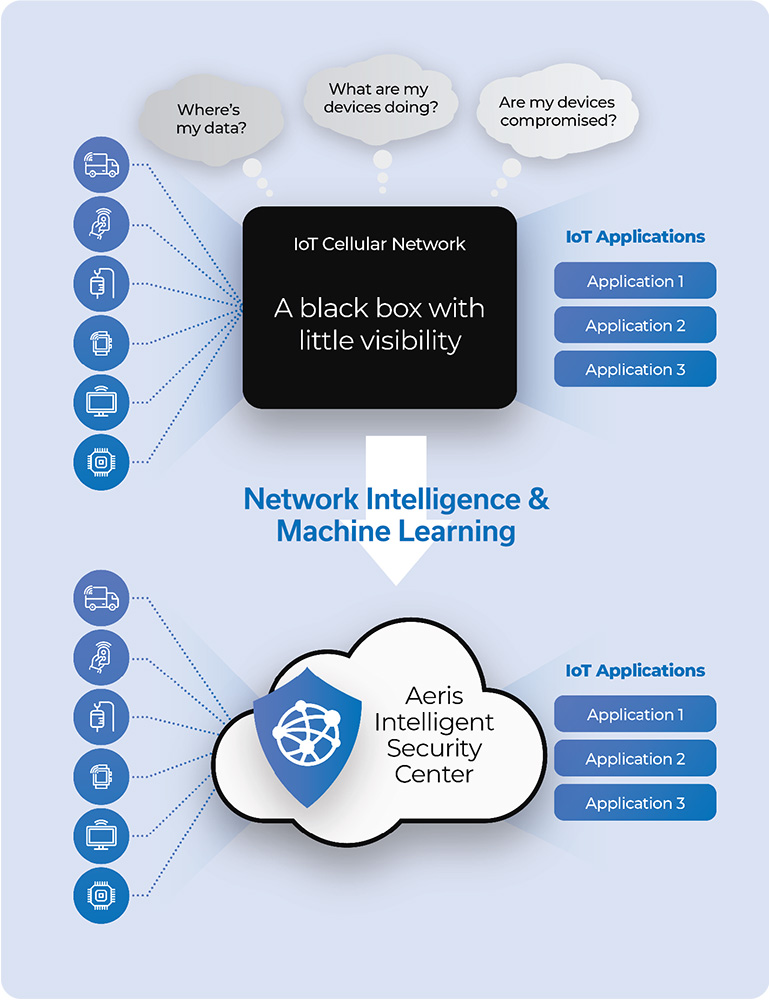
For those who have the old perception that a cellular network for your connected RPM devices is a “black box” and the security posture of your enterprise network ends at your enterprise firewall, think again. The Aeris Intelligent Security Center (AISC) is our latest offering that seamlessly integrates advanced network detection and response (NDR) capabilities with our intelligent cellular IoT network. It delivers harmonized, cost-effective, and easy-to-use cybersecurity to your connected RPM devices. This approach requires zero extra setup time while protecting your patient’s RPM device from day one. Having a single vendor that provides both connectivity and security helps streamline your IoT program and reduces the complexity of business logistics.
To learn more about AISC and how it harmonizes intelligent network security with IoT connectivity, enabling faster monetization of your connected medical devices with less risk and more predictability, check out our newest brochure about IoT security for RPM devices, or contact us for a product demo.